Key takeaways:
There are many over-the-counter (OTC) allergy medications. Popular categories include antihistamines, decongestants, and corticosteroids (steroids). You can find them as oral liquids and pills, eye drops, and nasal sprays.
Some OTC allergy medications, like decongestants, are meant for short-term use. Antihistamines relieve symptoms fast, while steroid nasal sprays can take a couple of weeks to work. But they both control chronic symptoms best when taken every day.
The best OTC allergy medication for you depends on your symptoms, health history, and other factors. Your prescriber or pharmacist can help you navigate your options.
Save on related medications
If you’re struggling with allergy symptoms, many effective allergy medications are available over the counter (OTC). Antihistamines, decongestants, and corticosteroid (steroid) nasal sprays are a few options. And you can find them in many combination products too.
Knowing how different OTC allergy medications work and what symptoms they treat can help you choose the best option for your needs.
Types of OTC allergy medications
The main types of OTC allergy medications are:
Decongestants
Steroid nasal sprays
Mast cell stabilizers
Search and compare options
Most types of OTC allergy medications come in more than one form, such as tablets, eye drops, and nasal sprays. They’re also often available in combination products that contain more than one type of medication for multisymptom relief.
Let’s take a closer look at each type of OTC allergy medication in greater detail.
Antihistamines
Antihistamines work by blocking histamine, a chemical released from your cells during an allergic reaction. Blocking histamine can reduce itchy eyes, sneezing, and a runny nose caused by allergies.
Antihistamines are available OTC as oral liquids, capsules, and tablets. Eye drops and nasal sprays are also available. Oral antihistamines have more body-wide effects compared with those used in your eyes or nose. Some of them can make you feel drowsy, while others are considered nondrowsy.
The different OTC antihistamines are listed in the table below.
Oral antihistamines | Antihistamine eye drops | Antihistamine nasal sprays |
|---|---|---|
Nondrowsy: Drowsy: | • Ketotifen (Zaditor, Alaway) | • Azelastine (Astepro) |
*May still cause drowsiness in some people
If you’re taking oral antihistamines to manage your allergy symptoms, experts recommend taking them every day — not just when your symptoms flare up. And starting them a few weeks before allergy season hits can help prevent symptoms in the first place.
Decongestants
Decongestants narrow blood vessels in the nasal passages, leading to decreased swelling. This temporarily relieves nasal congestion and sinus pressure. Certain decongestants are kept behind the pharmacy counter, but you can find others OTC, as shown in the table below.
Oral decongestants | Decongestant nasal sprays |
|---|---|
• Pseudoephedrine (Sudafed)* | • Oxymetazoline (Afrin, Dristan) |
*Available behind the counter or with a prescription, depending on where you live
Unlike antihistamines, decongestants aren’t meant for long-term use. You should take oral decongestants for only up to 7 days, unless directed by a healthcare professional. You shouldn’t use decongestant nasal sprays for more than 3 days in a row. Otherwise, your congestion may become harder to treat.
Pharmacist tip: Phenylephrine is another oral decongestant sold OTC. But it isn’t well absorbed when taken by mouth. And in 2023, the FDA found that oral phenylephrine isn’t effective for congestion. Many products containing this ingredient are no longer available. But it’s a good idea to check the OTC label and choose one of the above ingredients instead of oral phenylephrine if you’re looking for effective congestion relief.
Steroid nasal sprays
Steroid nasal sprays work by reducing swelling and inflammation inside your nasal passages and sinuses. This can help control sneezing, congestion, and a runny nose. Nasal steroid sprays can also help manage eye-related allergy symptoms. Compared with other OTC allergy medications, steroid nasal sprays tend to work the best for chronic allergy symptoms.
Examples of OTC steroid nasal sprays include:
Budesonide (Rhinocort Allergy)
Fluticasone (Flonase Allergy Relief, Flonase Sensimist)
Triamcinolone (Nasacort Allergy 24HR)
Mometasone (Nasonex 24HR Allergy)
It can take up to 2 weeks to get the full benefit from steroid nasal sprays. So it’s recommended to start a steroid nasal spray a few weeks before your allergies typically start. If you’re already experiencing allergy symptoms, adding an oral antihistamine for the first 2 weeks can help bridge the gap until the nasal spray starts to work.
Combination antihistamine and decongestant medications
You can also find antihistamines and decongestants combined in one pill, as well as in a combination eye drop.
Since many oral combination products contain pseudoephedrine, they’re typically located behind the pharmacy counter. Similar to nasal decongestants, you should limit combination eye drop use to no more than 3 days. If you use them for longer, your symptoms may get worse.
Common OTC combination allergy medications are shown in the chart below.
Oral combination medications | Combination eye drops |
• Cetirizine / pseudoephedrine (Zyrtec-D) |
Combination allergy products can be a convenient option. But you may end up taking additional ingredients that you don’t need. In other cases, you may accidentally double up on ingredients if you’re taking multiple products with the same ingredient. Check the active ingredients list on the OTC “Drugs Facts” label to be sure you aren’t doubling ingredients and that you’re taking medication only for symptoms you’re experiencing.
Mast cell stabilizers
Mast cell stabilizers work by acting on immune system cells responsible for triggering allergy symptoms. When used preventively, they can improve symptoms like swelling, sneezing, and runny nose. Only one mast cell stabilizer nasal spray is available OTC: cromolyn (NasalCrom).
Cromolyn nasal spray can take up to 6 weeks to feel its full effects. So it may not be the best choice if you need fast relief. And you need to use it more often than other nasal sprays for allergies — up to 6 times daily compared with once or twice a day. What’s more, cromolyn is likely less effective than steroid nasal sprays. But it may be a helpful option if you’re unable to tolerate nasal steroid sprays or they aren’t effective for you.
What is the best OTC allergy medication?
In general, experts recommend steroid nasal sprays as first-choice medications for people with chronic or severe allergies. But the best OTC allergy medicine for you can depend on your symptoms, health history, and other factors.
For example, certain allergy medicines may be preferred over others if you’re pregnant. Older adults should avoid antihistamines that cause drowsiness, such as diphenhydramine. And decongestants can have serious side effects if you have high blood pressure that’s uncontrolled.
You may also find that you get better relief when combining more than one type of OTC allergy medication, like an antihistamine nasal spray with a steroid nasal spray. But you should avoid combining multiple allergy medicines from the same class.
The graphic below compares the three common types of allergy medications based on dosage forms, side effects, costs, and more.
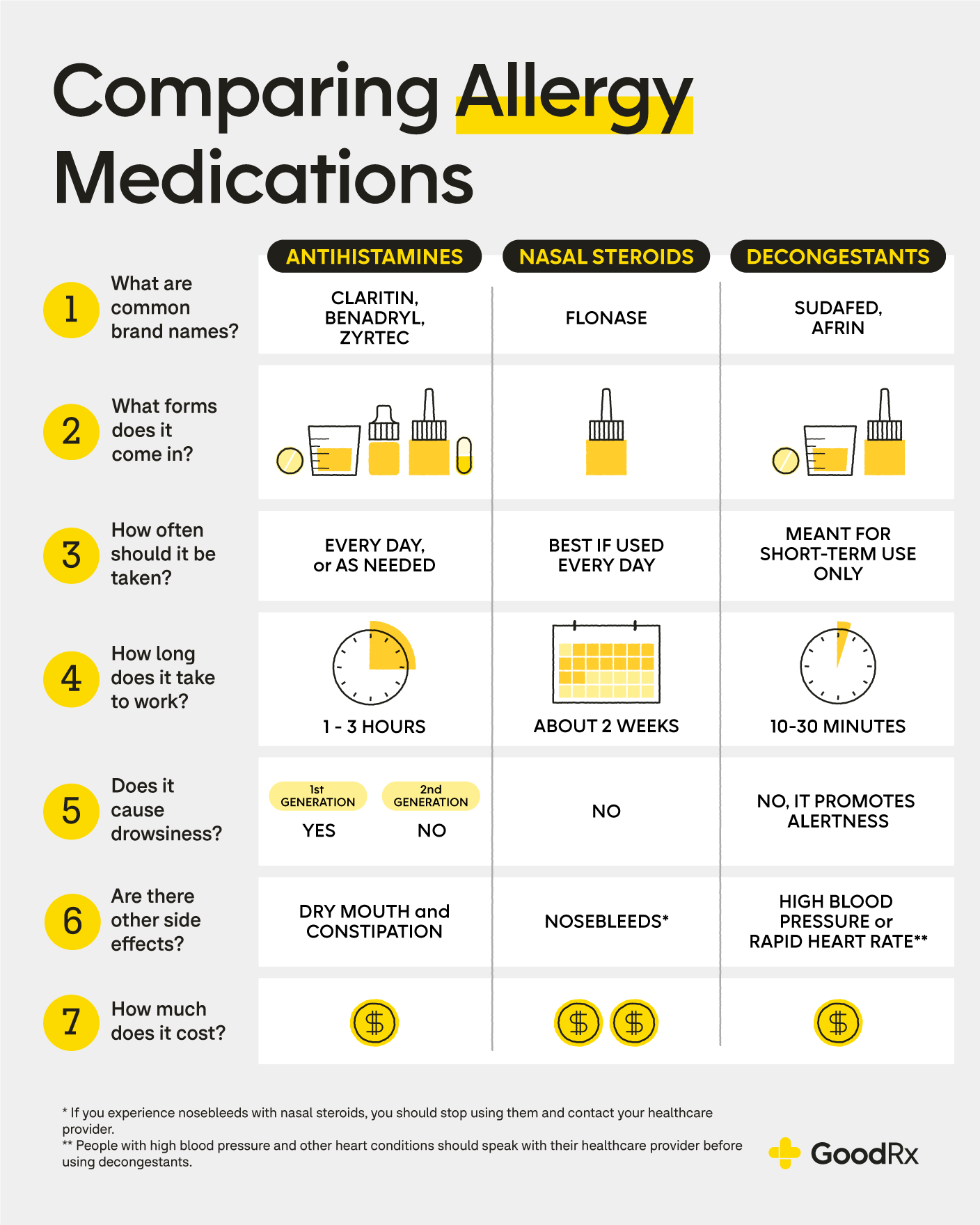
Still have questions? Your prescriber and pharmacist can help. They can be great resources to help you pick a safe and effective OTC allergy medication.
Prescription allergy medicines and treatments to consider
In addition to OTC allergy medications, there are many prescription medications for allergies. If OTC medications don’t work, talk to your prescriber. A prescription medication may be better for you. Examples of these include:
Dymista (azelastine / fluticasone) nasal spray
Ryaltris (olopatadine / mometasone) nasal spray
Patanase (olopatadine) nasal spray
Singulair (montelukast) tablets
Your healthcare team can also talk to you about other treatments. For example, allergy shots and a shot-free alternative called SLIT (sublingual immunotherapy) can help decrease allergic reactions in some people.
Frequently asked questions
Yes, most steroid nasal sprays and oral antihistamines are considered safe and effective options for allergies during pregnancy. But you shouldn’t use Nasacort or decongestants in most cases. Your prenatal care team can help you find the best allergy treatment for your needs.
It depends on what type of allergy medication you’re taking. Oral antihistamines, oral decongestants, and decongestant and antihistamine nasal sprays typically provide relief within a few hours or less. But steroid and mast cell stabilizer nasal sprays can take weeks to reach their full effect. In some cases, combining a fast-acting allergy medication with a slow-acting one can help you get the best symptom relief overall.
Yes, most steroid nasal sprays and oral antihistamines are considered safe and effective options for allergies during pregnancy. But you shouldn’t use Nasacort or decongestants in most cases. Your prenatal care team can help you find the best allergy treatment for your needs.
It depends on what type of allergy medication you’re taking. Oral antihistamines, oral decongestants, and decongestant and antihistamine nasal sprays typically provide relief within a few hours or less. But steroid and mast cell stabilizer nasal sprays can take weeks to reach their full effect. In some cases, combining a fast-acting allergy medication with a slow-acting one can help you get the best symptom relief overall.
The bottom line
There are many over-the-counter (OTC) allergy medications to choose from. They come as oral pills and liquids, eye drops, and nasal sprays. Antihistamines and steroid nasal sprays are popular options. But you may also find relief from decongestants and mast cell stabilizers. Combination products are also available for multisymptom relief.
The best OTC allergy medication for you depends on your symptoms, health history, and preferences. Discuss your options with your prescriber or pharmacist so you can find one that meets your needs and provides relief.

Why trust our experts?



References
Alcon Laboratories. (2024). Naphcon A- naphazoline hydrochloride and pheniramine maleate solution/ drops [package insert]. DailyMed.
Bausch & Lomb. (2023). Opcon-A - naphazoline hydrochloride and pheniramine maleate solution/ drops [package insert]. DailyMed.
Dykewicz, M. S., et al. (2020). Rhinitis 2020: A practice parameter update. The Journal of Allergy and Clinical Immunology.
Kenvue Brands. (2024). Visine allergy eye relief multi-action- naphazoline hydrochloride and pheniramine maleate solution/ drops [package insert].DailyMed.
MedlinePlus. (2017). Histamine: The stuff allergies are made of.
Seidman, M. D., et al. (2015). Clinical practice guideline: Allergic rhinitis. Otolaryngology–Head and Neck Surgery.
U.S. Food and Drug Administration. (2023). FDA clarifies results of recent advisory committee meeting on oral phenylephrine.















