Key takeaways:
Cataract surgery is one of the most common surgeries across the world.
Cataract surgery is very safe. But complications can happen, including corneal swelling, infection, macular edema, and a malpositioned lens.
Removing a cataract with cataract surgery can restore your vision.
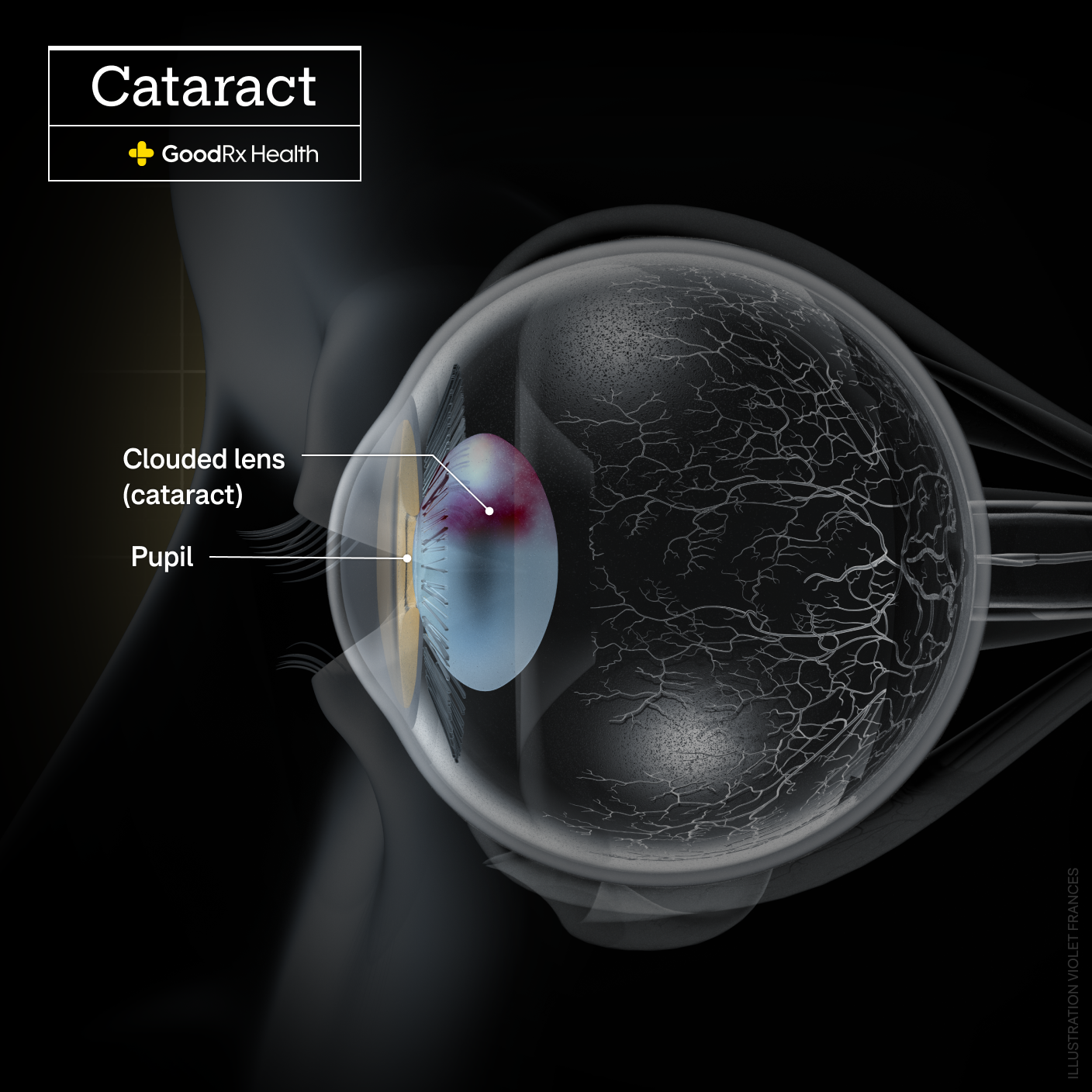
The lens of your eye is a clear disc that sits behind the pupil. The lens allows you to focus on objects. As you get older, the lens becomes cloudy and can develop into a cataract. And some children are born with cataracts.
Cataracts make it difficult to see. They cause blurred vision, glare, and trouble seeing at night.
If you have a cataract that’s affecting your vision, you may need cataract surgery to remove it. Cataract surgery is one of the most common surgeries in the U.S. and across the world. Ophthalmologists perform about 10 million cataract surgeries every year worldwide.
Search and compare options
Let’s take a look at cataract surgery and the most common questions people have as they prepare for surgery.
When do you need to have cataract surgery?
If cataracts are keeping you from doing important things — it’s time to have them removed.
You may need cataract surgery if you:
Can’t drive at night because of glare
Have trouble seeing even with your prescription glasses
Can’t finish work because of low vision
Have to skip social functions because of trouble seeing
If you have other eye conditions that affect your retina, like macular degeneration or diabetic retinopathy, you may need cataract surgery. Cataracts can make your lens so cloudy that it becomes impossible for your ophthalmologist to see your retina during an eye exam. So to check your retinal health, you’ll need to have cataracts removed.
What happens during cataract surgery?
During cataract surgery, an ophthalmologist makes small incisions in the eye and removes the lens. They remove the lens through phacoemulsification, a process that uses ultrasound energy to break up the lens so it’s easy to remove.
After removing the lens, they replace it with a clear, artificial lens that stays in your eye for the rest of your life.
Read more like this
Explore these related articles, suggested for readers like you.
Is cataract surgery different from LASIK?
Cataract surgery involves the lens, while LASIK or PRK involves the cornea (the clear outer portion of the eye). Some ophthalmologists use a laser during cataract surgery. Lasers are also part of LASIK and PRK surgery. That’s why the two procedures sometimes get confused.
Is cataract surgery painful?
You may feel some pressure during the procedure, but you shouldn’t feel pain because you’ll receive pain medication (anesthesia).
You have several options for anesthesia during cataract surgery, including:
Topical anesthesia with numbing eye drops
Local anesthesia, which involves injecting anesthetic medication around the eye
Sedation, during which you’ll receive medication through an intravenous (IV) line to relax
Most people do not need general anesthesia for cataract surgery. That means you’ll be awake during surgery, but you should feel comfortable and calm. If you feel pain or start feeling anxious during your surgery, let your ophthalmologist know right away. They can give you additional medication to make sure you’re comfortable.
How long does cataract surgery take?
Cataract surgery can take anywhere from 10 to 45 minutes, depending on your eye health. But you also need to factor in time for speaking to your doctor, receiving medications, and recovering from anesthesia. Your entire visit may take several hours.
Make sure to set up a ride home for after surgery. You probably won’t feel up to driving. And you won’t be allowed to drive if you receive certain types of anesthesia medications.
What do you need to do before cataract surgery?
You’ll need a full eye exam before surgery. You’ll also have tests to figure out which type of artificial lens is best for you.
There are many types of lenses, including standard and premium lenses. Standard lenses are the least expensive and often have fewer side effects. But if you use a standard lens, you’ll have to wear glasses to see close up after surgery if you have presbyopia.
Premium lenses can correct both distance and near vision, which can relieve symptoms of presbyopia. Premium lenses are more expensive and can have higher risk of side effects like glare. Talk to your doctor about your daily activities. They can help you figure out the best option for you.
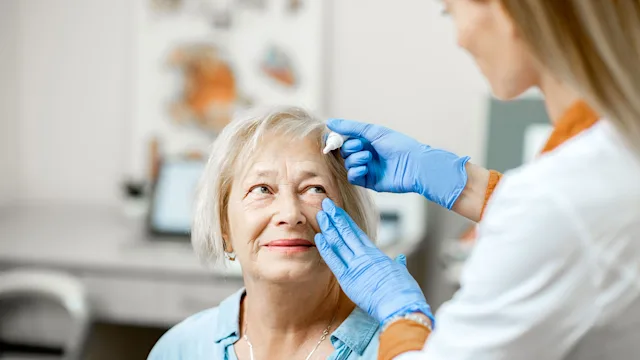
In addition to picking out your lens, you may need to use eye drops before surgery. You’ll also want to get ready for life after surgery. It’s helpful to review some post-cataract surgery recovery tips before your procedure.
How long does it take to recover from cataract surgery?
Every eye heals differently. But in general the recovery period from cataract surgery is short. The good news is that within a few days you’ll be almost back to yourself.
Most people feel back to normal within 1 month, but the full recovery can take up to 3 months.
Do cataracts grow back?
Cataracts do not grow back.
But sometimes a few cells from the top layer of the natural lens can remain after cataract surgery. As these cells grow and divide over time, they develop into a membrane that covers the artificial lens. This is a secondary cataract, or posterior capsular opacification.
If the secondary cataract affects your vision, your doctor may recommend a YAG capsulotomy, a laser procedure to remove it.
Do you need glasses after cataract surgery?
Depending on the type of intraocular lens you choose, you may need glasses after cataract surgery.
If you choose a standard lens, you’ll likely need glasses to either correct for distance or near vision. If you choose a multifocal lens, you may not need glasses unless reading very small print.
Can you see right after cataract surgery?
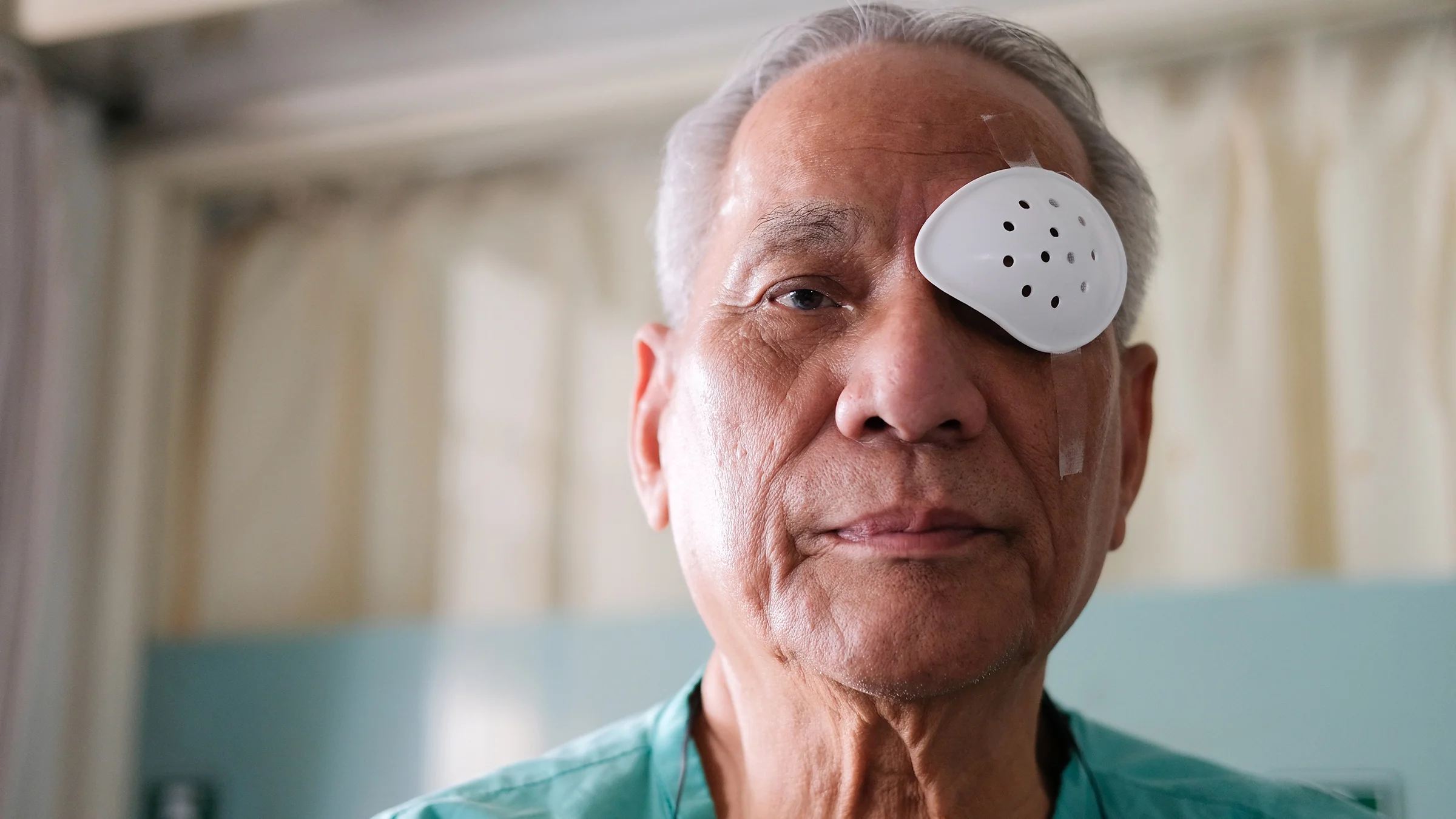
You may notice that your vision is improved right after surgery. But if you don’t, that’s OK.
Most of the time ophthalmologists recommend that you cover your eye with a patch for a day. After you remove the patch, your vision may take a few days to clear up. But it can take a few weeks for some people.
Even if it takes longer than you expect, rest assured, your vision will be much clearer in the end. Your ophthalmologist may prescribe eye drops for you to use after surgery. These drops can help speed up healing so your vision clears faster.
What is the most common complication of cataract surgery?
Secondary cataract is one of the most common complications after cataract surgery. It’s so common that most ophthalmologists don’t refer to it as a complication at all. That’s because it’s almost impossible to guarantee that surgery will remove all lens cells.
Otherwise, the most common complication is macular swelling, or cystoid macular edema. This usually occurs about 6 to 8 weeks after surgery. Your ophthalmologist may recommend monitoring, eye drops, or injections to help remove this fluid.
The bottom line
Cataracts cause low vision and develop as you age. Cataract surgery can be a life-changing procedure that restores vision. It’s a short, low-risk surgery that removes the lens of the eye and replaces it with an artificial lens. Most people recover from cataract surgery very quickly. Complications include secondary cataracts and macular swelling, which your ophthalmologist can treat.

Why trust our experts?


References
Awasthi, N., et al. (2009). Posterior capsular opacification: A problem reduced but not yet eradicated. Archives of Ophthalmology.
Boyd, K. (2022). What is a posterior capsulotomy? American Academy of Ophthalmology.
Foster, A. (2000). Vision 2020: The cataract challenge. Community Eye Health.
Gurnani, B., et al. (2021). Phacoemulsification. StatPearls.
Pesudovs, K., et al. (2003). Refractive error changes in cortical, nuclear and posterior subcapsular cataracts. British Journal of Ophthalmology.
Randolph, J., et al. (2019). Cataract surgery complications. EyeWiki.
Schein, O. D., et al. (2000). Anesthesia management during cataract surgery: Summary. AHRQ Evidence Report Summaries.