Key takeaways:
Stevens-Johnson syndrome (SJS) is a rare skin reaction. The cause is usually a new medication.
SJS often begins with flu-like symptoms, such as fever, chills, muscle aches, and fatigue.
Skin symptoms of Stevens-Johnson syndrome include a rash that turns into blisters. These can lead to extensive skin peeling that can put you at risk of dehydration and infection.
SJS needs emergency medical treatment, which includes controlling the symptoms, preventing complications, and addressing the underlying cause.
Stevens-Johnson syndrome (SJS) is a rare but serious skin condition. The most common cause is a reaction to a medication. SJS causes the skin to get inflamed, blister, and peel. The blistering can cover large parts of the body. If more than 30% of the body is affected, it’s called toxic epidermal necrolysis (TEN).
Even though the skin symptoms are most noticeable, SJS can also cause dangerous inflammation in other organs. And the blistering puts people at risk for serious complications, like dehydration and infection. So SJS is a medical emergency that needs prompt diagnosis and treatment to prevent long-term harm.
What are the symptoms of Stevens-Johnson syndrome?
SJS typically develops within 1 to 3 weeks after starting a medication. It can also start after someone has stopped taking a certain medication (usually within 2 weeks).
Search and compare options
Early signs of SJS
SJS usually starts with flu-like symptoms, such as:
Sore throat
Fever
Body aches
Cough
These are the signs of early-stage Stevens-Johnson syndrome. In this stage, most people aren’t aware that their symptoms are from SJS. This is especially true because the symptoms are similar to what you may feel at the start of a cold or the flu.
Other signs and symptoms
More than 90% of people with SJS will also have mucosal involvement, which means that the mucus membranes are affected. The eyes are the most commonly affected, but the genitals, airway, and throat can all be affected as well. Symptoms include:
Burning or stinging in the eyes
Eye discharge or crusting
Sensitivity to light
Pain with urination (peeing)
Shortness of breath
Sores or blisters inside the mouth
Difficulty swallowing
SJS rash
The SJS rash often starts 1 to 3 days after the other symptoms. And as the rash evolves, it can change in appearance and location from day to day. Here’s the common progression of the SJS rash:
It typically first appears on the upper chest, face, and the hands and feet.
When it first starts, the rash looks like red, purple, or brown spots of different sizes.
The spots then become darker in the middle and lighter around the edges. These are sometimes called “target” lesions because they look like a bull’s-eye.
Within hours to days, it starts to spread to other parts of the body. Most often it spreads to the abdomen, arms, and legs.
As it spreads, the red spots join together and form fluid-filled blisters.
The blisters eventually burst and the skin begins to peel. This exposes large areas of skin and creates a risk of infection.
The rash can be very painful, especially when the skin starts to blister and heal. When this happens, it can also lead to dehydration and skin infections.
What does the SJS rash look like?
Here are some Stevens-Johnson syndrome rash pictures to help you know what it looks like.
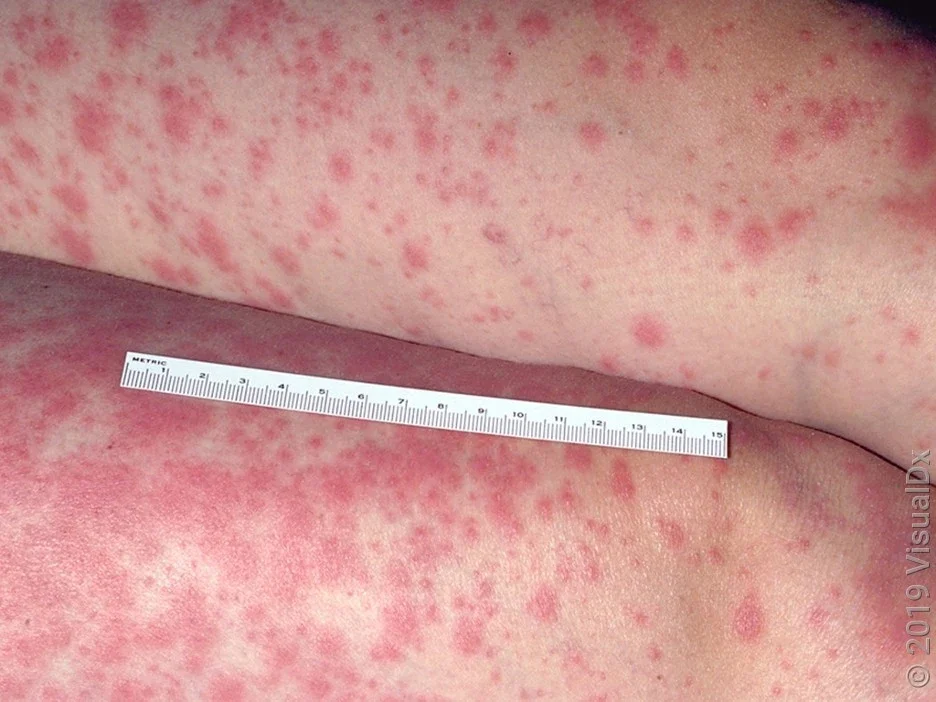

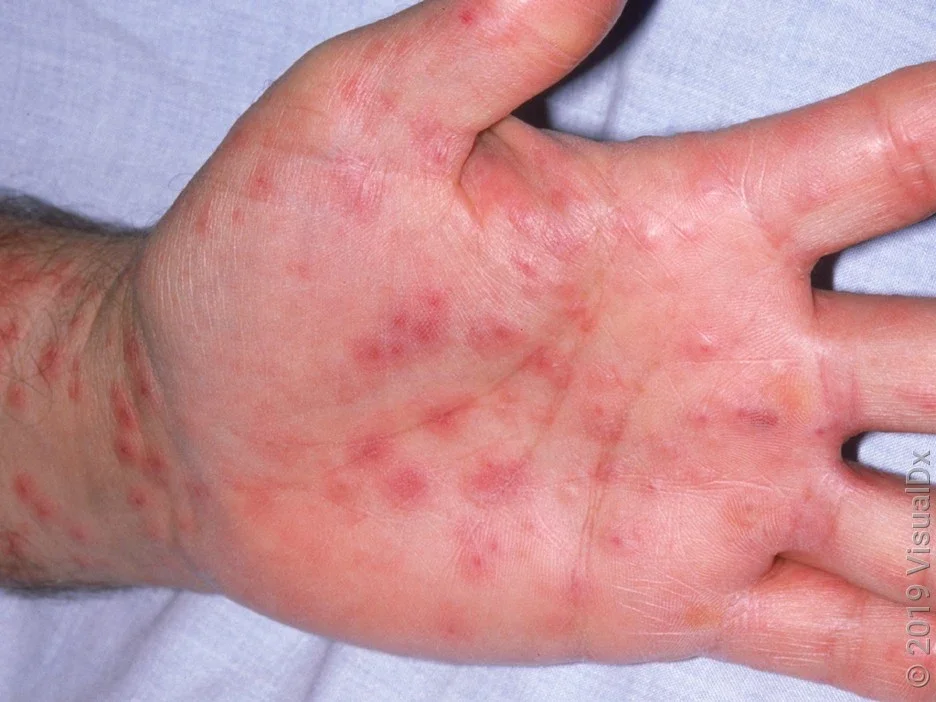
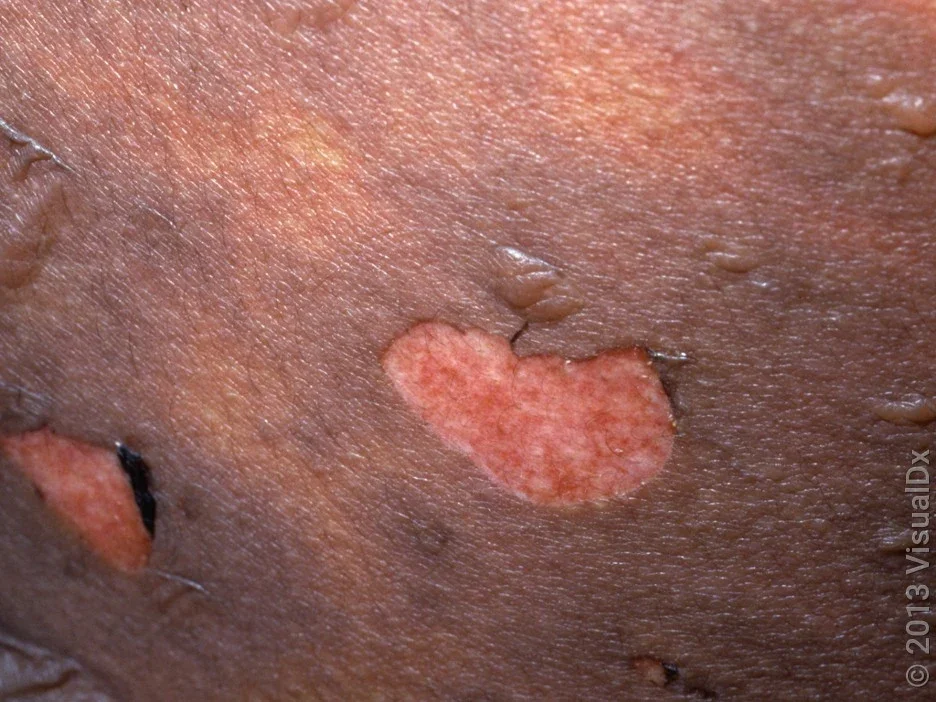
What causes Stevens-Johnson syndrome?
The most common cause of SJS is a reaction to a medication that someone has taken. But other causes (like infections) are also possible. Here’s an overview of the different causes of SJS.
Read more like this
Explore these related articles, suggested for readers like you.
Medications that can cause SJS
More than 100 medications can cause SJS. Most often these include:
Sulfa medications: zonisamide, sulfamethoxazole / trimethoprim (Bactrim), sulfasalazine
Antibiotics: ampicillin, amoxicillin, cephalosporins, fluoroquinolones
Anti-seizure medications: carbamazepine, lamotrigine, phenobarbital, phenytoin
Allopurinol: a medication that treats gout and kidney stones
Pain relievers: nonsteroidal anti-inflammatory drugs (NSAIDs), like diclofenac and ibuprofen (Advil, Motrin), and acetaminophen (Tylenol)
Teriflunomide: a medication that treats multiple sclerosis (MS)
Here’s a more complete list of the different medications that have been connected to cases of SJS.
Infections that can cause SJS
A less common cause of SJS is an actual infection. Examples of infections that can do this are:
Mycoplasma pneumonia: Another name for this pneumonia is “walking pneumonia,” because it doesn’t cause severe symptoms. It’s more commonly associated with SJS in children and teens.
Cytomegalovirus (CMV): This common virus can affect people of any age. It generally doesn’t cause any symptoms unless a baby is born with it.
Human immunodeficiency virus (HIV): This virus attacks the body’s immune system.
Herpes simplex virus (HSV): This virus often causes sores on the mouth or genitals.
Epstein-Barr virus (EBV): This virus commonly spreads through saliva. It often leads to infectious mononucleosis, or the “kissing disease.”
Influenza virus: This common infection affects the nose, throat, and lungs.
Coxsackievirus: This virus causes a rash in children, often on their hands, feet, and in their mouth, hence its popular name, hand, foot, and mouth disease. In adults, it can cause symptoms like the common cold.
Less common causes of SJS
SJS might occur for other reasons, too. For example, there have been a few cases of people developing SJS after receiving a vaccination. But these reports are rare, and it isn’t clear if the vaccine itself led to SJS.
Other rare causes of SJS include graft-versus-host disease, a condition that can develop after a bone marrow or organ transplant. And sometimes SJS develops for no known reason.
Diagnosis for Stevens-Johnson syndrome
A healthcare professional can often diagnose SJS just by looking at your skin and reviewing your symptoms. The appearance of the rash and the way it spreads helps make the diagnosis of SJS.
What tests are used to diagnose Stevens-Johnson syndrome?
To confirm the diagnosis, a healthcare professional may do a skin biopsy. They’ll take a small sample of skin and look at it under a microscope.
Treatment for Stevens-Johnson syndrome
SJS can be life-threatening when the blistering leads to some of the complications we discussed above. So early recognition and treatment are important.
Treatment for SJS is best in the hospital because SJS creates a risk of dehydration and infection. Severe cases may need treatment in a burn unit because they’re equipped to handle skin peeling and wound care.
Since a medication reaction causes most cases of SJS, the most important first step in treating SJS is stopping that medication.
A key part of treatment for SJS is supportive and specialized medical care. This includes:
Intravenous (IV) fluids to maintain hydration
Daily wound care with nonadhesive dressings
Pain relief medications
High-calorie food to promote healing
Specialized eye care if SJS affects the eyes or eyelids
Antibiotics in the case of skin infection
Some cases need additional treatments. The decision depends on the severity of SJS and if the underlying cause is unknown. These treatments may include:
Cyclosporine: Cyclosporine may decrease how long SJS lasts.
Plasmapheresis: This can help remove parts of the harmful medication from the blood.
TNF blockers: Tumor necrosis factor (TNF)-alpha inhibitors can decrease inflammation.
Steroids: Corticosteroids may improve outcomes if started early.
Immunoglobulin infusion: Intravenous immunoglobulin (IVIG) can block the medications from harming the body.
Can Stevens-Johnson syndrome be prevented?
Stevens-Johnson syndrome can’t be completely prevented since it’s not possible to know which medications you may react to. Having said that, here are some steps you can take to minimize the chances of getting SJS:
Notify a healthcare professional right away if you develop any type of skin rash after starting a new medication.
If a certain medication caused SJS or any serious skin rash in the past, avoid using that medication for the rest of your life.
Before starting certain higher-risk medications (like allopurinol), talk with your primary care provider about a simple blood test to see if you’re genetically more likely to develop a serious skin reaction.
When to see a healthcare professional
Stevens-Johnson syndrome is a medical emergency. Get medical attention if you think you have SJS or notice any of the following symptoms after starting a new medication:
Have unexplained body aches or tiredness
Develop a red, purple, or brown rash that spreads
Have any pain or soreness in your eyes, throat, or genitals
Develop any blisters or open sores
Keep in mind that medications can cause many different types of skin reactions, and most of them aren’t serious. If you develop a reaction, a healthcare professional can help you figure out the cause and next steps.
Frequently asked questions
About 10% of people with Stevens-Johnson syndrome will die from it. This can happen from different complications, like:
Pneumonia
Bacterial infection leading to sepsis (a blood infection)
Organ failure
The first symptoms of SJS usually begin within 4 weeks of starting a new medication. The rash starts a few days after the initial symptoms and it usually lasts about 8 to 12 days.
Some rashes can look similar to SJS, but they have different causes and treatments. So, getting the right diagnosis early is important. Examples include:
About 10% of people with Stevens-Johnson syndrome will die from it. This can happen from different complications, like:
Pneumonia
Bacterial infection leading to sepsis (a blood infection)
Organ failure
The first symptoms of SJS usually begin within 4 weeks of starting a new medication. The rash starts a few days after the initial symptoms and it usually lasts about 8 to 12 days.
Some rashes can look similar to SJS, but they have different causes and treatments. So, getting the right diagnosis early is important. Examples include:
The bottom line
Stevens-Johnson syndrome (SJS) is a well-known condition that can be quite scary. The blistering is extensive, and few skin conditions can lead to such life-threatening complications. But keep in mind that it’s very rare. With early detection and good wound care, people can make a full recovery. It’s important to be aware of the risks of any medication before you start taking it, but the likelihood you’ll develop SJS from one of them is low.

Why trust our experts?



Images used with permission from VisualDx (www.visualdx.com).
References
Benedetti, J. (2024). Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN). Merck Manual Professional Version.
Boston Children’s Hospital. (n.d.). Staphylococcal scalded skin syndrome (SSSS) in children.
Cheng, L. (2021). Current pharmacogenetic perspective on Stevens-Johnson syndrome and toxic epidermal necrolysis. Frontiers in Pharmacology.
Ergen, E. N., et al. (2017). Stevens-Johnson syndrome and toxic epidermal necrolysis. JAMA Dermatology.
Fakoya, A. O. J., et al. (2018). Stevens-Johnson syndrome and toxic epidermal necrolysis; extensive review of reports of drug-induced etiologies, and possible therapeutic modalities. Open Access Macedonian Journal of Medical Sciences.
Frantz, R., et al. (2021). Stevens-Johnson syndrome and toxic epidermal necrolysis: A review of diagnosis and management. Medicina.
Justiz, A. A., et al. (2024). Graft-versus-host disease. StatPearls.
King, C. (2022). Erythema multiforme. DermNet.
MedlinePlus. (2020). Stevens-Johnson syndrome/toxic epidermal necrolysis.
MedlinePlus. (2025). Skin biopsy.
National Organization for Rare Disorders. (2024). Stevens-Johnson syndrome and toxic epidermal necrolysis.
Ngan, V., et al. (2016). Stevens-Johnson syndrome / toxic epidermal necrolysis. DermNet.
Schneider, J. A., et al. (2017). Stevens-Johnson syndrome and toxic epidermal necrolysis: A concise review with a comprehensive summary of therapeutic interventions emphasizing supportive measures. Advances in Therapy.
Shanbhag, S. S., et al. (2020). Multidisciplinary care in Stevens-Johnson syndrome. Therapeutic Advances in Chronic Disease.
Yao, L. M., et al. (2025). Recent developments in the research of Stevens-Johnson syndrome and toxic epidermal necrolysis: pathogenesis, diagnosis and treatment. European Journal of Medical Research.
Zimmerman, D., et al. (2019). Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN): Immunologic reactions. Oncologic Critical Care.


















