Key takeaways:
The best way to protect yourself from measles is to know your vaccination status and ensure you — and your loved ones — are fully immune.
Full immunity requires two doses of the MMR (measles, mumps, and rubella) vaccine, given at least 28 days apart. For most people, this provides lifelong protection.
If you’re not immune, there are still steps you can take after exposure. One option is to get the MMR vaccine within 3 days to help prevent infection.
Stay informed about local outbreaks. Measles spreads easily and quickly. If you think you’ve been exposed, contact a healthcare professional right away.
Save on related medications
Imagine finding out someone at a party or school event had measles. What should you do next?
With measles cases popping up across the U.S., it’s natural to feel concerned — especially if you’re unsure about your or your child’s protection. Knowing the basics about how measles spreads, what symptoms to watch for, and how to lower your risk can go a long way in helping you feel prepared.
In this article, we’ll walk through what you need to know — including six practical tips from healthcare professionals to help you and your family stay protected.
1. Review your vaccination records
Many people aren’t sure whether they’ve had the measles vaccine — and that’s OK. Most adults in the U.S. are protected against measles — either because they were vaccinated as children or because they were exposed to the virus naturally before vaccines became widely available.
For adults
A good first step is to check your immunization history. Your parent, pharmacist, doctor, or local health department can help you find your records or figure out the next best steps if your vaccination status is unclear. If you can’t access your records, a simple blood test can show if you have immunity to measles.
For children
If you’re a parent, it’s also a good idea to double-check your child’s records, especially if they’re approaching school age or haven’t had a recent well-child visit. Staying up to date on the measles vaccine helps protect your child and your community.
2. Stay up to date with the measles vaccine (MMR or MMRV)
Vaccination is the most effective way to prevent measles. There are two measles vaccines available in the U.S.:
MMR vaccine (measles, mumps, and rubella): It’s available as MMR II and Priorix for adults and children ages 12 months and older.
MMRV vaccine (measles, mumps, rubella, and varicella/chickenpox): It’s available as ProQuad for children between 12 months and 12 years.
You can get the MMR or MMRV vaccine at a doctor’s office, pharmacy, or health department. It’s OK to have questions or concerns, and healthcare professionals are there to help with these.
For adults
Most adults are considered protected, but if you don’t have documentation of receiving two doses of the measles vaccine and don’t have a lab test showing immunity, you should get vaccinated. It’s better (and safer) to be re-vaccinated than to not be vaccinated.
International travel
If you’re planning international travel and you think you need a measles vaccine, it’s a good idea to book a medical visit at least 6 weeks in advance to allow time for vaccination and full protection before your trip.
For high-risk situations
Some people have a higher risk of exposure to measles, or a higher risk of severe illness. For example, during an outbreak, in healthcare settings, or if you’re immunocompromised. In these cases, it’s especially important to have two documented doses of the measles vaccine at least 28 days apart, or a lab test that shows immunity.
For pregnancy
If you’re pregnant or planning to become pregnant, the measles vaccine isn’t given during pregnancy. But it’s safe and recommended beforehand if you’re not yet immune.
For children
The CDC recommends two doses of the measles vaccine as part of the routine childhood vaccine schedule:
First dose at 12 to 15 months
Second dose at 4 to 6 years
One dose is about 93% effective at preventing measles. Two doses increase that protection to about 97%.
If your child missed one or both doses, it’s not too late to catch up. For example, if they receive their first dose at age 7, they can get their second dose at least 28 days later.
For international travel or during outbreaks
In some cases, children may be advised to get the MMR vaccine earlier than usual. For example, if there’s a local measles outbreak or if you’re planning to travel internationally with your infant, your medical team may recommend a dose between ages 6 and 11 months.
This early dose provides short-term protection but doesn’t count toward the routine two-dose series — so your child will still need two more MMR doses later (at 12-15 months and 4-6 years).
3. Know what to do if you’re exposed
If you think you’ve been exposed to measles, it’s important to act quickly — especially if you’re not sure whether you’re protected. Early steps can help limit the transmission and may even prevent you from getting sick.
Contact your doctor’s office or pharmacist right away: They can assess your risk, check your immunization status, and report the exposure to your local health department if needed. This helps with testing, monitoring, and preventing further transmission.
Check your vaccination and immunity status: Look through your health records — or your child’s — to see if you’ve had the MMR vaccine or a confirmed measles infection in the past. Or, arrange a blood test. If you have documentation of vaccination, measles infection, or your blood test shows you’re immune, you’re likely protected and don’t need further treatment.
Take steps to prevent transmitting measles: If you’re not immune — or your status is unclear — it’s safest to isolate to help protect others. This is especially important if you spend time around young children, pregnant women, and people with a weak immune system. So avoid schools, day care centers, workplaces, and crowded settings during your isolation period.
Ask about postexposure treatment: If you’re not immune, there are still ways to lower your chances of getting sick. Typically, this involves a dose of the measles vaccine within 3 days (72 hours) of exposure. But in some cases, a treatment called immunoglobulin (an injection of antibodies) can be given within 6 days of exposure to protect high-risk people like infants younger than 6 months, pregnant women, or those with weakened immune systems.
4. Stay informed during outbreaks
Measles cases can pop up quickly — especially in communities with lower vaccination rates or high rates of international travel. Stay in the loop by checking local health department updates or asking your pharmacist if there’s any measles activity in your area. Being aware helps you take timely precautions.
5. Practice good hygiene and reduce exposure
Measles spreads through the air and can linger in a room even after a person with the infection leaves.
Regular handwashing and covering coughs and sneezes is always good practice. This helps reduce the spread of many illnesses — including measles.
If you live near a measles outbreak, try to limit time in crowded indoor spaces and keep your distance from anyone who’s sick.
6. Talk to a doctor, pharmacist, or other trained medical professional about your concerns
If you’re unsure about your risk or have questions about the measles vaccine, you’re not alone. Healthcare professionals like pharmacists and doctors are there to support you — not to pressure or judge. They can help you understand your options and guide you toward choices that feel right for you and your family.
What is measles?
Measles is a highly contagious viral illness that affects the respiratory system. It’s caused by the measles virus and can lead to serious health complications, especially in children and people with weakened immune systems.
Even just a few measles cases can trigger an outbreak, particularly in communities where vaccination rates have dropped. That’s why early prevention and public awareness are key to keeping measles under control.
How is measles transmitted?
Measles spreads extremely easily — it’s one of the most contagious respiratory illnesses. You can catch measles through:
Respiratory droplets from coughing or sneezing
Direct contact with a person with the infection
Touching contaminated surfaces and then touching your face
The virus can stay in the air or on surfaces for up to 2 hours, and people can pass it before they even feel sick.
Although measles was declared eliminated in the U.S. in 2000, outbreaks have increased in recent years due to declining vaccination rates.
When fewer people are vaccinated, the risk of transmission increases. Staying up to date with vaccines helps protect those who can’t get vaccinated — like infants and people with weakened immune systems.
If you have questions or concerns about the MMR vaccine, your pharmacist or doctor can talk you through the facts and help you feel more confident in your choices.
What are the symptoms of measles?
Measles starts like other viral illnesses. Symptoms similar to a common cold or virus usually appear 1 to 2 weeks after you’re exposed to someone with measles:
High fever
Runny nose
Cough
Red, watery eyes
Small white spots inside the mouth (called Koplik spots)
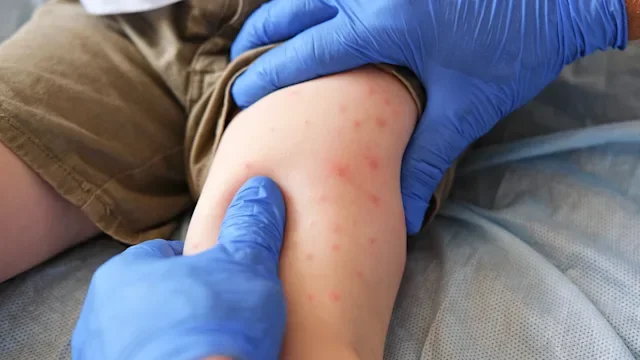
What does the measles rash look like?
What sets measles apart from other viral infections is the rash, which appears about 3 to 5 days after symptoms begin. It typically starts as flat red spots at the hairline, then spreads to the face, and moves down the body. In people with darker skin tones, the spots may be harder to see.


Measles complications
While many people recover, measles can cause serious complications like:
Pneumonia, in about 1 in 20 children with measles
Brain swelling (encephalitis), in about 1 in 1,000 children
And in rare cases, measles can be life-threatening.
Who is most at risk for measles?
Certain groups are more likely to get sick or experience complications if exposed to measles, including:
Unvaccinated children and adults
Infants under 12 months who are too young for the routine MMR vaccine
People with weakened immune systems
Travelers visiting countries with lower vaccination rates or active measles outbreaks
Frequently asked questions
The MMR vaccine provides long-lasting protection. After two doses, most people are protected for life and don’t need a booster.
It’s rare, but not impossible. Because one dose of the MMR vaccine is about 93% effective, and two doses are about 97% effective, this means a small number of vaccinated people might still get measles. But, their symptoms are often milder, and complications are less likely.
Getting vaccinated not only protects you — it also helps protect others. When enough people are vaccinated, it creates herd immunity, which helps shield those who can’t get vaccinated, like babies younger than 6 months and people with weakened immune systems.
Most people don’t experience any side effects from the MMR vaccine. When they do happen, they’re usually mild and go away on their own. These may include:
Soreness at the injection site
Low-grade fever
Mild rash
Temporary joint pain (more common in adults)
Serious side effects are extremely rare. One persistent misunderstanding is that the MMR vaccine causes autism — but this has been thoroughly disproven by several large-scale studies. The vaccine is safe, effective, and widely recommended by major medical organizations all over the world.
The MMR vaccine provides long-lasting protection. After two doses, most people are protected for life and don’t need a booster.
It’s rare, but not impossible. Because one dose of the MMR vaccine is about 93% effective, and two doses are about 97% effective, this means a small number of vaccinated people might still get measles. But, their symptoms are often milder, and complications are less likely.
Getting vaccinated not only protects you — it also helps protect others. When enough people are vaccinated, it creates herd immunity, which helps shield those who can’t get vaccinated, like babies younger than 6 months and people with weakened immune systems.
Most people don’t experience any side effects from the MMR vaccine. When they do happen, they’re usually mild and go away on their own. These may include:
Soreness at the injection site
Low-grade fever
Mild rash
Temporary joint pain (more common in adults)
Serious side effects are extremely rare. One persistent misunderstanding is that the MMR vaccine causes autism — but this has been thoroughly disproven by several large-scale studies. The vaccine is safe, effective, and widely recommended by major medical organizations all over the world.
The bottom line
You don’t have to navigate measles concerns on your own. Whether you’re up to date on vaccinations or still weighing your options, there are steps you can take today to protect yourself, your family, and your community.
The MMR (measles, mumps, and rubella) vaccine remains the most effective way to prevent measles. The CDC recommends two routine doses for young children, but it’s also important for certain adults to confirm their immunity — especially during an outbreak or before international travel. Infants, too young for the routine series, may benefit from early vaccination in some situations.
If you’re exposed to measles, contact a medical care provider promptly and follow their guidance to help prevent the virus from spreading.

Why trust our experts?



Images used with permission from VisualDx (www.visualdx.com).
References
Centers for Disease Control and Prevention. (2022). Traveling with children.
Centers for Disease Control and Prevention. (2024). Catch-up immunization schedule for children and adolescents.
Centers for Disease Control and Prevention. (2024). About handwashing.
Centers for Disease Control and Prevention. (2024). Measles vaccine recommendations.
Centers for Disease Control and Prevention. (2024). Measles symptoms and complications.
Centers for Disease Control and Prevention. (2024). Plan for travel.
Centers for Disease Control and Prevention. (2025). Chapter 7: Measles.
Centers for Disease Control and Prevention. (2025). Clinical overview of measles.
Centers for Disease Control and Prevention. (2025). Global measles.
Centers for Disease Control and Prevention. (2025). Measles cases and outbreaks.
Centers for Disease Control and Prevention. (2025). Measles vaccination.
Merck, Sharpe and Dohme. (2023). Proquad- measles, mumps, rubella and varicella virus vaccine live injection, powder, lyophilized, for suspension [package insert].
Novilla, M. L. B., et al. (2023). Why parents say no to having their children vaccinated against measles: A systematic review of the social determinants of parental perceptions on MMR vaccine hesitancy. Vaccines.
Pietrantonj, C. D., et al. (2020). Vaccines for measles, mumps, rubella, and varicella in children. Cochrane Database of Systematic Reviews.
World Health Organization. (2024). Measles.