Key takeaways:
Eczema is a chronic skin condition that shares some similarities with autoimmune skin diseases.
By strict definition, eczema isn’t an autoimmune disease.
There’s a close link between eczema and autoimmune diseases. In fact, if you have one, you’re more likely to develop the other.
The immune system is involved in eczema flare-ups, so medications that target the immune system are helpful in controlling symptoms.
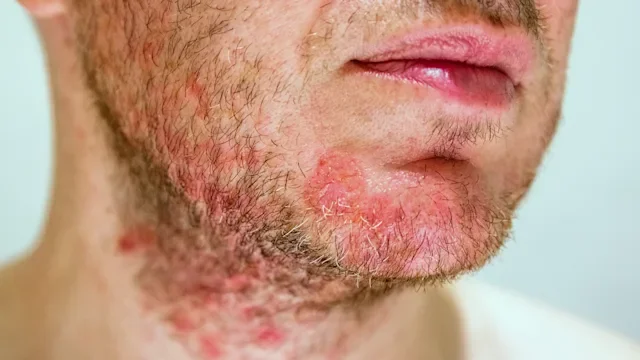
Eczema is a chronic skin condition that causes skin inflammation, itching, and a rash. Atopic dermatitis is the most common type of eczema (and the focus of this article). It affects people of all ages, but it’s especially common in children. The symptoms can range from very mild to severe. For many, these can be intense enough to disrupt sleep, daily routines, and quality of life.
Experts don’t know the exact cause of eczema. It likely develops from a mix of genetics, environmental exposures, and an overactive immune system. That’s why many people wonder: Is eczema an autoimmune disease?
Eczema and autoimmune conditions do share some similarities. And researchers are still trying to understand how the two are linked. Despite the overlap, eczema isn’t considered an autoimmune disease. Understanding why can help you make sense of your symptoms and your treatment options.
Search and compare options
What is an autoimmune disease?
An autoimmune disease is a condition where your immune system mistakenly targets healthy cells in your own body. This attack can happen in your skin or the organs inside your body.
Normally, the immune system has a great filter to know what in the body belongs and what doesn’t. For example, when you get sick, your immune system can find the germ and destroy it. The immune system also has a memory. So, if you get the same bug again, it may recognize it faster.
But sometimes the immune system doesn’t work properly. Instead of targeting an intruder, it mistakenly targets healthy parts of your own body.
For example, Type 1 diabetes is an autoimmune disorder. In this condition, the immune system attacks specific cells in the pancreas that help make insulin. When these cells are destroyed, the pancreas can no longer make insulin — leading to the lifelong need for insulin replacement.
Is eczema an autoimmune disease?
The simple answer is: No, eczema isn’t an autoimmune disease. But the two conditions are closely linked. In eczema, the immune system isn’t attacking a specific target in the skin or the body. This is a key feature that defines an autoimmune disease.
That said, there are certain parts of the immune system that may be overactive in eczema, leading to an itchy rash. These are called “inflammatory factors.” That’s why certain medications that suppress the immune system also help improve eczema.
Are any forms of eczema considered autoimmune diseases?
Other types of eczema are also not considered autoimmune diseases. Here’s a brief look at these:
Allergic contact dermatitis happens when your skin develops an allergy to something it comes into contact with (like nickel).
Irritant contact dermatitis happens when your skin gets irritated by something it comes into contact with (like chemicals).
Nummular dermatitis usually develops on the arms or legs, and it may be related to dry or sensitive skin.
Seborrheic dermatitis (dandruff) is an overreaction to a yeast that normally lives on the skin.
Are people with autoimmune conditions more likely to develop eczema?
Research shows that people with autoimmune conditions are more likely to develop eczema. This is especially true of autoimmune conditions involving the skin and gastrointestinal system. The more autoimmune diseases you have, the stronger the risk.
Examples of conditions that may increase your risk of eczema include:
Inflammatory bowel disease (like Crohn’s disease or ulcerative colitis)
And this is a two-way connection. People with eczema are also more likely to develop certain autoimmune disorders, like:
Inflammatory bowel disease (like Crohn’s disease or ulcerative colitis)
Vitiligo
Hypothyroidism
Alopecia areata
What causes eczema?
An overactive immune system is only part of the story when it comes to developing eczema. Other factors also play a role.
Genetic factors
A genetic cause for eczema may occur when a part of the skin — filaggrin — doesn’t work properly. Filaggrin plays a role in the skin’s defense against intruders. It’s part of the skin barrier at the surface of the skin. It acts like a glue to help keep things out of the skin and to keep moisture in.
Altered skin barrier
When filaggrin isn’t working properly, the skin barrier falls apart. This can lead to:
An inability to keep skin moist
Very dry skin
An easy entry for irritants, allergens, and bacteria
These effects can lead to chronic eczema flares and inflammation in the skin.
Environmental factors
Environmental causes can lead to eczema that develops or worsens in adulthood. These eczema causes include:
Skin irritants (detergents or heavy fragrances)
Allergens (pet dander or dust)
Very dry or cold air
Overwashing
When should you see a healthcare professional about eczema?
If you notice signs of eczema or any skin changes, schedule a checkup with your primary care provider or dermatologist. And if you have a history of autoimmune conditions, be sure to let your healthcare team know. This can help them figure out if you have eczema or another skin condition, such as ringworm, psoriasis, or scabies.
There are many treatments for eczema that work well to manage symptoms. From medications to home remedies, a healthcare professional can help you figure out the next best steps.
Frequently asked questions
No, eczema isn’t contagious. There’s no way to “catch it” from someone else. Eczema is the result of genetic and environmental factors and an overactive immune system.
No, there’s no cure for eczema. But keep in mind that there are many treatment options that work well to lessen symptoms and keep your skin clear.
Yes, dry and cold air can lead to eczema flares, which can feel very itchy. In the U.S., these weather conditions tend to happen in the winter season. You can help prevent winter eczema flare-ups on your hands by:
Wearing gloves when you go outside
Washing your hands only when necessary
Using thick moisturizer frequently
Yes, eczema is considered an inflammatory disease, and there’s a connection between eczema and inflammation. This is because people with eczema tend to have increased levels of certain immune cells (or inflammatory cells). This is why anti-inflammatory medications work to treat eczema. They lower the levels of those cells.
No, having eczema doesn’t mean that you’ll develop an autoimmune disease. You may have an increased risk of developing certain autoimmune conditions (like vitiligo or alopecia areata). But it doesn’t mean that you will.
No, eczema isn’t contagious. There’s no way to “catch it” from someone else. Eczema is the result of genetic and environmental factors and an overactive immune system.
No, there’s no cure for eczema. But keep in mind that there are many treatment options that work well to lessen symptoms and keep your skin clear.
Yes, dry and cold air can lead to eczema flares, which can feel very itchy. In the U.S., these weather conditions tend to happen in the winter season. You can help prevent winter eczema flare-ups on your hands by:
Wearing gloves when you go outside
Washing your hands only when necessary
Using thick moisturizer frequently
Yes, eczema is considered an inflammatory disease, and there’s a connection between eczema and inflammation. This is because people with eczema tend to have increased levels of certain immune cells (or inflammatory cells). This is why anti-inflammatory medications work to treat eczema. They lower the levels of those cells.
No, having eczema doesn’t mean that you’ll develop an autoimmune disease. You may have an increased risk of developing certain autoimmune conditions (like vitiligo or alopecia areata). But it doesn’t mean that you will.
The bottom line
Eczema involves inflammation and an overactive immune response, but it isn’t considered an autoimmune disease. That’s because genetics and environmental triggers also play major roles. Still, the two are strongly connected. People with eczema have a higher risk of autoimmune conditions, and people with autoimmune conditions are more likely to develop eczema. But one doesn’t turn into the other.

Why trust our experts?



References
Brown, S. J., et al. (2012). One remarkable molecule: Filaggrin. Journal of Investigative Dermatology.
Cipriani, F., et al. (2017). Autoimmune diseases involving skin and intestinal mucosa are more frequent in adolescents and young adults suffering from atopic dermatitis. The Journal of Dermatology.
de Lusignan, S., et al. (2022). Atopic dermatitis and risk of autoimmune conditions: Population-based cohort study. The Journal of Allergy and Clinical Immunology.
DermNet. (n.d.). Irritant contact dermatitis.
Ivert, L. U., et al. (2021). Association between atopic dermatitis and autoimmune diseases: A population-based case-control study. The British Journal of Dermatology.
Lu, Z., et al. (2021). Atopic dermatitis and risk of autoimmune diseases: A systematic review and meta-analysis. Allergy, Asthma & Clinical Immunology.
National Eczema Association. (2025). Nummular eczema.