Key takeaways:
Eczema and eczema rashes aren’t contagious. You can’t get eczema from touching someone who has it.
People with eczema are more likely to get skin infections. The germs that cause those infections can sometimes spread through contact.
Frequent hand washing, avoiding direct contact, and not sharing objects can lower the risk of developing a contagious rash.
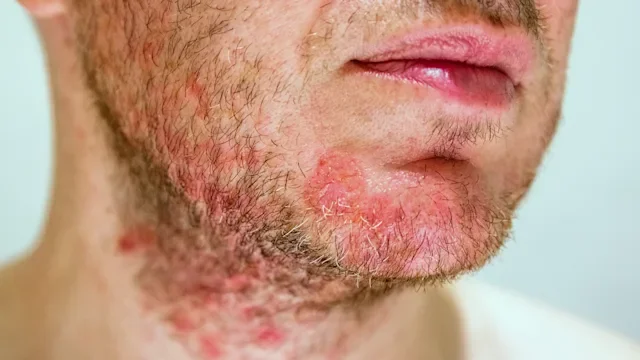
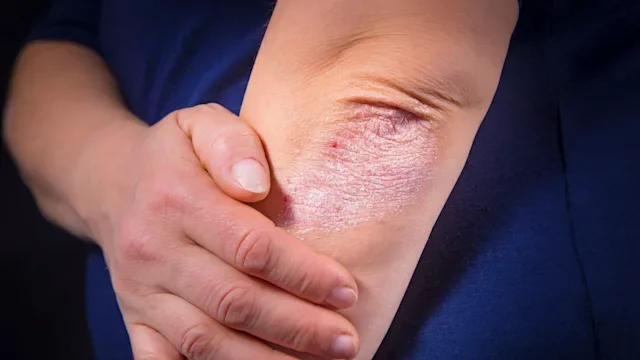
Eczema can look uncomfortable — and sometimes alarming. This often leads to one big question: Is eczema contagious?
Here’s how eczema works, plus when rashes are safe to be around and what steps can lower the risk of spreading contagious skin infections.
Is eczema contagious?
Eczema isn’t contagious. Eczema is an inflammatory condition that’s caused by immune system and skin-barrier changes. These changes can’t be passed from one person to another through touching, kissing, or sharing objects.
Are eczema rashes contagious?
An eczema rash isn’t contagious. You won't develop eczema if you come in contact with someone having an eczema flare. An eczema rash can’t move from person to person. But people with an eczema flare are more likely to develop certain skin infections. The germs that cause these infections are contagious. Let’s take a closer look.
Impetiginized eczema
Impetigo is a skin infection caused by the bacteria Staphylococcus aureus. This bacteria lives on your skin. It’s harmless unless it enters your body. It can enter your skin and cause impetigo if you have a break in your skin from a wound or rash.
Eczema flares damage the natural skin barrier. This increases the risk for infections like impetigo.
Staphylococcus aureus can pass from person to person through touch. Coming in contact with this rash doesn’t mean you’ll definitely develop impetigo. But it can increase your risk. So it’s best to wash your hands often. Also, avoid touching the rash and sharing objects with people who have impetigo.
Fungal infections
People with eczema flares are also at higher risk for some fungal skin infections, like ringworm and skin candidiasis (yeast infections).
These fungi can live on your skin. They’re harmless — unless they manage to get past the skin barrier’s protective defenses through breaks or inflammation in the skin.
Fungi can pass from person to person through touch. Coming in contact with these germs doesn’t mean you’ll definitely get ringworm or a yeast infection. But it can increase your risk.
It’s best to wash your hands often and avoid touching the rash or sharing objects with people who have a fungal skin infection.
Eczema herpeticum
The herpes simplex virus (HSV) is a very common and contagious virus that causes cold sores and genital herpes.
People with eczema can develop eczema herpeticum. This is a condition where the herpes virus infects inflamed skin. Eczema herpeticum is very painful and can cause serious illness. Many people with eczema herpeticum need hospital-based treatment.
HSV can pass from person to person through touch. You won’t develop eczema herpeticum if you come in contact with the rash. But can develop other types of HSV infections, like cold sores.
Avoid touching the rash or sharing objects with people who have eczema herpeticum. Make sure to wash your hands often if your loved one has eczema herpeticum.
What causes eczema?
It’s not clear what causes eczema.
Genes affect a person’s risk of developing eczema. Most people with eczema have family members who also have eczema. Children are much more likely to develop eczema if their parents have eczema too. So, eczema isn’t contagious, but it's hereditary.
The environment also plays a role in eczema. Certain exposures can cause eczema flares.
The skin’s microbiome can also play a role. A healthy skin microbiome seems to lower the risk of developing eczema.
What makes eczema rashes spread?
Eczema rashes can start on one part of the body and then spread. This can happen for many reasons.
Eczema can get infected with bacteria, viruses, and fungi. These germs can spread to other parts of your body and cause infections. To lower the risk of spreading infections to other parts of your body, here are some things to do:
Start treatment for the infection as soon as possible.
Keep the area covered.
Avoid touching the area as much as possible.
Wash your hands after applying any treatment to the area.
Wash your hands any time you touch the area.
Eczema flares can also get worse and affect more parts of the body. This doesn’t mean the area is infected. But it does mean that inflammation is getting worse. To lower the risk of flare getting worse, here’s what to keep in mind:
Avoid flare triggers.
Use your eczema medications and treatments as prescribed by your healthcare team.
Use gentle soaps and detergents.
Moisturize regularly.
When should you seek care for eczema?
Many eczema flares can be treated at home using your flare treatment plan. But some flares need extra medical care. Talk with your healthcare team right away in these cases:
You’re using your treatment plan, and your symptoms are getting worse.
Your skin is very red or painful.
You develop blisters or skin swelling.
You develop a fever or feel unwell.
The skin around areas of eczema flare are red, painful, or swollen.
You develop red streaking on your arms or legs.
The bottom line
Eczema can look alarming, which is why it’s common to worry about whether it can spread to others. Eczema itself isn’t contagious. But damaged skin during a flare can make infections more likely. The germs that cause these infections can pass from person to person.
You can help keep flares and infections under control. Pay attention to changes in the skin. Also, get medical advice when symptoms worsen.

Why trust our experts?


References
De Bruyn Carlier, T., et al. (2021). Autoreactive T cells and their role in atopic dermatitis. Journal of Autoimmunity.
Eichenfield, L. F., et al. (2014). Guidelines of care for the management of atopic dermatitis: Section 1. Diagnosis and assessment of atopic dermatitis. Journal of the American Academy of Dermatology.
Lopez, D. J., et al. (2021). Association between ambient air pollution and development and persistence of atopic and non-atopic eczema in a cohort of adults. Allergy.
National Eczema Association. (2021). The human skin microbiome and its changes in atopic dermatitis.
National Eczema Society. (2021). Skin infections and eczema.
National Health Service. (2024). Atopic eczema.
Thomsen, S. F., et al. (2007). Importance of genetic factors in the etiology of atopic dermatitis: A twin study. Allergy and Asthma Proceedings.
Xiao, A, et al. (2024). Eczema herpeticum. StatPearls.