GoodRx Guide
What Is Hepatitis A? Causes, Symptoms, and Treatment
Comprehensive information for you or a loved one — including treatment options and discounts on popular medications.Definition
Hepatitis A is an infection that causes liver inflammation and swelling. Hepatitis A is caused by the hepatitis A virus (HAV).
Many people who get HAV feel sick for weeks to months but then get better. Some people develop long-term liver damage and liver failure. It’s rare, but some people have died from hepatitis A.
What causes hepatitis A to spread?
Hepatitis A spreads from person to person when the virus gets into someone’s mouth. Hepatitis A is very contagious. Even tiny amounts of the virus can cause infection.
People with hepatitis A release the virus in their stool. This is called viral shedding. The virus can then easily spread from hands to surfaces, food, or drinks — even when someone tries to be careful about cleanliness.
You can get exposed when you do the following:
Touch a contaminated surface, and then eat, drink, or prepare food without washing your hands.
Share utensils, drinks, or food with someone who has hepatitis A.
Eat food handled or prepared by someone who has hepatitis A.
Eat food that has been contaminated with the hepatitis A virus.
Drink water or another liquid that has been contaminated with the hepatitis A virus.
Have close personal or sexual contact with someone who has hepatitis A.
Share needles with someone who has hepatitis A.
Certain situations increase your chances of being exposed to the virus:
Close personal or sexual contact increases exposure. Spending a lot of time with someone who has hepatitis A raises the chance of coming into contact with the virus. This happens through shared surfaces, food, or physical contact. This increased exposure also increases the risk of getting hepatitis A.
Travel to certain countries can also raise your risk. Hepatitis A is more common in certain parts of the world. You’re more likely to get exposed to hepatitis A when you’re in a place where the virus is more common.
How is hepatitis A diagnosed?
Several pieces of information help diagnose someone with hepatitis A:
Hepatitis A blood test: The main blood test for hepatitis A looks for a specific antibody called IgM anti-HAV. When this antibody is present in your blood, it means you have a recent or active hepatitis A infection.
Liver function tests: Liver function tests are blood tests that show signs of liver inflammation or injury. These tests offer clues on how hepatitis A is affecting your liver health.
Stool samples: Stool tests can sometimes detect the hepatitis A virus. They’re usually only helpful during certain early stages of infection.
Symptoms and history: Your symptoms aren’t enough to confirm the infection, but they can help your healthcare team decide which tests to order. Information about your travel, food exposures, or close contacts can also offer important clues.

What are the symptoms of hepatitis A?
Symptoms of hepatitis A infection include:
Fever
Fatigue
Nausea and vomiting
Stomach pain
Diarrhea
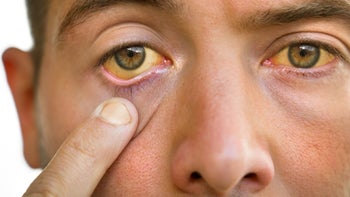
Yellow color of the eyes and skin (jaundice)
Stools that are light in color
Joint pain
Symptoms usually start about 1 month after exposure to the virus and tend to come on suddenly. They can last for several weeks to months and gradually go away.
Most people with hepatitis A develop a mild illness. And some never develop symptoms.
But some people with hepatitis A develop more serious complications like:
Relapsing hepatitis: About 15% of people develop relapsing hepatitis or gallbladder disease. During a relapse, people experience symptoms of hepatitis A, but the symptoms are usually more mild. People are contagious during the relapse.
Acute liver failure: Acute liver failure is a rare but serious complication of hepatitis A. Fewer than 1% of people with hepatitis A develop liver failure. But about 1 in 3 people who develop liver failure from hepatitis A die or need a liver transplant.
How do you treat hepatitis A?
There’s no cure for hepatitis A. And there’s no medication that directly treats the virus. Treatment focuses on easing symptoms and supporting your overall health while your body recovers.
This can include:
Rest
Hydration
Ibuprofen (Advil, Motrin) to help with fever
Medication to help with nausea and vomiting
Avoiding alcohol, medications, and vitamins that put stress on the liver
Once you recover, you’re immune to hepatitis A for life.
How can you prevent hepatitis A?
There are several things you can do to protect yourself against hepatitis A.
1. Get vaccinated against hepatitis A
Vaccination is the best way to protect yourself from getting hepatitis A. The hepatitis A vaccine is a 2-dose vaccine series given 6 months apart.
Anyone can request a hepatitis A vaccine. It’s safe for adults, children, and infants over 12 months old. Consider getting vaccinated if you:
Travel to areas where hepatitis A outbreaks are common
Work in day care or healthcare settings
Have chronic liver disease or have a liver transplant
2. Take steps to protect yourself while traveling
If you’re traveling to an area where hepatitis A is common, you can lower your risk by taking these protections:
Get vaccinated at least 2 weeks before travel.
Wash your hands often and before eating or preparing food.
Drink bottled, sealed water or water that has been boiled. Avoid tap water, ice made from tap water, and fountain drinks.
Use bottled or boiled water to brush your teeth.
Eat fully cooked foods. Avoid raw fruits and vegetables unless you peel them yourself.
Avoid unpasteurized products
3. Seek medical care if you come in contact with hepatitis A
You should contact your healthcare team right away if you think you may have been exposed to hepatitis A. Exposure can happen if you:
Live with or have close contact with someone who was diagnosed with hepatitis A
Ate food linked to a hepatitis A outbreak
Traveled to an area with a known hepatitis A outbreak
Were notified by a public health department about a possible exposure.
Your healthcare team may recommend treatment hepatitis A immunoglobulin. Hepatitis A immunoglobulin can keep you from getting sick with HAV — but only if you take it soon after exposure and before symptoms start.
Frequently asked questions
Hepatitis A outbreaks happen when many people in a community are not protected against the virus. This can occur when vaccination rates are low or when people haven’t had a past infection that gave them immunity.
Outbreaks are more likely in places where access to clean water and reliable sanitation is limited. The virus can spread more easily through food, drinks, and shared surfaces in these situations. Because hepatitis A spreads easily, it can move quickly through a community in these situations.
Hepatitis A is less common in the U.S. because more people are vaccinated and sanitation systems are widely available. But outbreaks can still happen, especially in areas where vaccination rates are low.
You should stay home from work or school as soon as you start having symptoms or find out you have hepatitis A. You’ll need to isolate yourself at home for at least 1 to 2 weeks.
Here are things to do while you’re sick:
Don’t prepare food for other people.
Avoid having sex.
Wash your hands with soap and water. Alcohol-based hand rubs won’t kill hepatitis A.
Clean your toilet often.
Don’t share towels.
Wash your clothes and laundry in hot water and separately from others’.
Clean surfaces with household bleach.
Hepatitis A can pass from person to person through sexual activity. Certain sex practices, like anal sex, can increase the likelihood of passing hepatitis A to someone else. That’s why health experts recommend not having sex when you have hepatitis A.
Two doses of the hepatitis A vaccine provide long-term — and likely lifelong — protection against the hepatitis A virus. Studies suggest that protection lasts at least 30 to 40 years. Many experts believe it may last even longer.
Hepatitis is a general term for liver inflammation. Many things cause hepatitis, including:
Infections
Medications
Alcohol
Medical conditions
Some of these things are curable while others aren’t. There’s no cure for hepatitis A. But most people recover from the illness after a few weeks and don’t develop long-term complications from this illness.
References
Centers for Disease Control and Prevention. (2024). Clinical screening and diagnosis for hepatitis A.
Centers for Disease Control and Prevention. (2025). 2026 CDC Yellow Book.
Centers for Disease Control and Prevention. (2025). Hepatitis A basics.
Fiore, A. E., et al. (2006). Prevention of Hepatitis A through active or passive immunization: Recommendations of the advisory committee on immunization practices (ACIP). Morbidity and Mortality Weekly Report.
Koenig, K. L., et. al. (2017). Hepatitis A virus: Essential knowledge and a novel identify-isolate-inform tool for frontline healthcare providers. Western Journal of Emergency Medicine.
National Health Service. (2026). Hepatitis A.
Nelson, N. P., et al. (2020). Prevention of hepatitis A virus infection in the United States: Recommendations of the advisory committee on immunization practices, 2020. Morbidity and Mortality Weekly Report.
NYC Health. (n.d.). Hepatitis A.
Shin, E. C., et al. (2018). Natural history, clinical manifestations, and pathogenesis of Hepatitis A. Cold Spring Harbor Perspectives in Medicine.
Shingina, A., et al. (2023). Acute liver failure guidelines. The American Journal of Gastroenterology.
World Health Organization. (2019). Hepatitis.